
Q&A: Tips for health and safety at the workplace in the context of COVID-19, published by the World Health Organisation (WHO) on 26 June 2020, has revealed how the leaden-footed UN agency has neither the knowledge nor the capacity to advise on issues of work.
But that has not stopped it for one moment. Omissions in its guide – notably no mention of labour inspection and enforcement, and a lack of awareness of potential interactions with other workplace hazards, and the necessity for wider employment protections – exposed why a non-workplace UN agency should not be leading on a workplace issue.
The WHO’s guidance contradicts far more protective guidance published in May 2020 by the UN’s specialist workplace agency, the International Labour Organisation (ILO).
The WHO Q&A repeats policy positions elaborated in its 10 May 2020 interim guide, Considerations for public health and social measures in the workplace in the context of COVID-19’. This document received a hostile reception, described by the International Trade Union Confederation (ITUC) and the Council of Global Unions as ‘dangerous’.
Miscalculated risk
WHO’s first blunder is a repeated assertion that “Covid-19 spreads primarily through respiratory droplets or contact with contaminated surfaces.” But concerns were raised early in the pandemic that droplet and contact risks were not the only threat posed by this coronavirus.
A paper published on 17 March 2020 in the New England Journal of Medicine noted the possibility for its far more extensive spread “since the virus can remain viable and infectious in aerosols for hours and on surfaces up to days”.
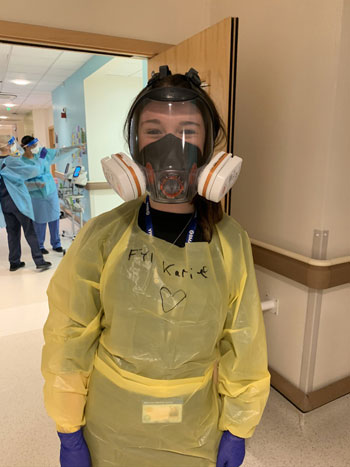
MASKED PROBLEM The World Health Organisation (WHO) has refused to recommend respirators for most health care workers, instead calling for far less protective medical or surgical masks.
Evidence of a wider airborne/aerosol transmission risk, putting workers in more jobs, more circumstances and at greater distances at risk, accumulated quickly.
A 1 June 2020 Lancet commentary accompanying a WHO commissioned review that contradicted WHO recommendations on key elements of its advice, including recommending much wider user of respirators by health care staff, notes: “Both experimental and hospital studies have shown evidence of aerosol transmission of SARSCoV2.”
It wasn’t WHO’s only blindspot. Paper after paper reported those infected but never displaying symptoms (asymptomatic) or not yet displaying symptoms (presymptomatic) were a significant source of infections.
WHO though continued to claim this mode of transmission was ‘very rare’. It assumed, without supporting evidence, Covid-19 behaved like its cousin severe acute respiratory syndrome (SARS) and other coronaviruses.
WHO had messed up. A 17 June 2020 paper published in the Lancet Infectious Diseases journal indicated the coronavirus that causes Covid-19 – also known as SARS-CoV-2 – spreads far more easily than either SARS or Middle East Respiratory Syndrome (MERS), with “substantial infectivity” during the incubation period. In a linked comment, Dr Virginia Pitzer from Yale School of Public Health noted the “findings confirm the relative importance of pre-symptomatic transmission.”
Without wider use of the correct PPE, apparently healthy individuals can transmit the coronavirus in workplaces, widely and unchecked. Aerosol transmission happens because the virus can fill a room or travel on a breeze. It’s just WHO can’t see it.
Transmission impossible
WHO’s mistakes and denials continue to inform its workplace guidance.
“The risk of exposure to Covid-19 in the workplace depends on the likelihood of coming within 1 metre of others, in having frequent physical contact with people who may be infected with Covid-19, and through contact with contaminated surfaces and objects,” it asserted in the 26 June Q&A.
Only that’s not what the evidence says. An expert review for the UK government published on 23 June 2020 noted: “There is evidence that the risk of transmission increases by 2-10 times at 1m compared to 2m and the potential for higher occupancy at 1m distancing will also increase risk if there are no mitigations.”
The UN’s specialist workplace agency, ILO – which unlike WHO has a dedicated workplace safety unit and liaises as a matter of course with employers and unions – recommends 2m.
A 22 June 2020 Stirling University commentary on the evidence on physical distancing noted the arguments for a 1m rule “do not stack up.” It added: “The science for lowering the 2m distance… appears to be limited if not absent.”
It was only on 7 July 2020, after an open letter signed by over 200 scientists from around the world and published in the journal Clinical Infectious Diseases, urged the WHO to airborne’ transmission that WHO acknowledged this may be a problem. It’s workplace guidance, though, remains unchanged.
Aiming low
WHO defines workers in its ‘low risk’ category as those with “minimal occupational contact with the public and other co-workers. Examples of such jobs may include remote workers (ie. working from home), office workers without frequent close contact with others and workers providing teleservices.”
Call/contact centre clusters provide a reality check on WHO’s assumption about white collar risks. A Strathclyde University survey of UK call centre workers found high levels of concern about exposure risks; 47.2 per cent ‘strongly agreed’ and 30.7 per cent ‘agreed’ with the statement, ‘I think it is likely that I will catch Covid-19’.
It appears their fears were well-founded. On 20 July, health officials said they were investigating an outbreak of coronavirus at an NHS test and trace call centre in Scotland. Sitel, which carries out contact tracing for the NHS, said it was aware of a “local outbreak” at its Motherwell site. By 21 July, it had been confirmed 15 workers were infected. Dave Moxham, deputy general secretary of the Scottish national union federation STUC, said it had been pointing out for months that call centre and similar office environments present a high Covid health and safety risk. “Statements from Sitel workers suggesting social distancing was not maintained during breaks and in shared spaces is obviously a particular concern,” he said.
A large call centre cluster in Korea affected 94 of the 216 workers on one floor (43.5 per cent). An April 2020 report in the Emerging Infectious Diseases journal noted that “alarmingly”, the outbreak “exemplifies the threat posed by SARS-CoV-2 with its propensity to cause large outbreaks among persons in office workplaces.”
Wrong on risks
“Jobs or tasks with close, frequent contact with the general public or others,” are ranked as medium risk by WHO, “where physical distancing of at least 1 metre may be difficult to observe, or tasks that require close and frequent contact between co-workers.” Examples “may include frontline workers in retail, home deliveries, accommodation, construction, police and security, public transport, and water and sanitation.”
However, Office for National Statistics figures published on 26 June 2020, analysing Covid-19 deaths in England and Wales by occupation up to 25 May 2020, revealed high rates in males in 17 occupations including taxi drivers and chauffeurs (135 deaths), security guards (107 deaths), and bus and coach drivers (54 deaths).
These are ‘medium risk’ in WHO’s ranking. According to ONS, in men “two major groups of occupations were found to have similarly high rates of death involving Covid-19. The first was elementary workers with 39.7 deaths per 100,000 men (421 deaths).

BRUSH OFF Cleaners are in one of the UK’s highest risk jobs for Covid-19, official figures show. WHO’s guidance, though, doesn’t recognise this and leaves them largely unprotected.
“The occupations in this group include those performing mostly routine tasks, such as construction workers and cleaners. The second was caring, leisure and other service occupations (39.6 deaths per 100,000 men, or 160 deaths), which include occupations such as nursing assistants, care workers and ambulance drivers.”
For women, a statistically significant excess was found in “caring, leisure and other service occupations,” which had a rate of 15.4 deaths per 100,000 women, equivalent to 264 deaths.
The same concentration of cases in certain job categories has been observed elsewhere, with new additions as workplaces reopen and clusters develop, notably in meat processing.
A study of work-related Covid-19 infection patterns in Asia, authored by experts from Harvard University’s TH Chan School of Public Health and published online on 19 May 2020, rated the top five jobs for infection risk as healthcare workers (HCWs), drivers and transport workers, services and sales workers, cleaning and domestic workers and public safety workers.
High risk strategy
In WHO’s ranking, high risk is limited to “jobs or tasks with close contact with people who may be more likely to have Covid-19, as well as contact with objects and surfaces possibly contaminated with the virus.”
Real-life tells are different story. Low wages, job insecurity and a rushed return to work – announced by UK prime minister Boris Johnson on 10 May 2020, the day before ONS first identified what unions described as ‘horrifying’ Covid-19 death rates in ordinary jobs – have made many varied workplaces the primary coronavirus frontline.
The process of getting to and from work on a crowded commute and navigating a workplace where your colleague might be little more than arm’s length away, creates the potential for lengthy exposures to a high number of people – two top risk factors for infection.
The infections that raced through meat processing plants in Germany, the UK, USA and many other countries affecting tens of thousands, were not the result of jobs that required workers to encounter those known to be infected in care or other settings, but the result of workers unwittingly or unavoidably – through fear of being fired or poverty – taking the virus to work. The evidence of concealed symptoms or presymptomatic or asymptomatic individuals entering the workplace is downplayed or dismissed by WHO.
WHO, what, how, why?
WHO ignores the large social class skew in coronavirus risk – broadly speaking, the lower your social class, the higher your risk.
Whole sections of the workforce potentially at risk as a result of discrimination and job segregation - including informal, insecure and women workers, Black and minority ethnic workers and migrant workers - are invisible in WHO’s risk assessment.
A study published on 10 June 2020 by the US National Employment Law Project concluded: “Our results suggest that virus transmission in the workplace may be exacerbated by employer repression and that the disproportionate impact of Covid-19 on Black communities may be related to greater exposure of Black workers to repressive workplace environments.”

RACISM KILLS Studies have shown more black and minority workers are employed in jobs with a high Covid-19 risk. Frances O’Grady, general secretary of the UK Trades Union Congress said: “Rather than just warm words, the government must now show that Black Lives Matter with action to protect black and minority ethnic (BME) people at work and to give all key workers the pay rise they have earned. BME communities must have confidence that their health is being taken seriously.”
The 26 June ONS update noted that of the 17 specific occupations in England that had increased death rates, 11 had a high proportion of black and ethnic minority workers. An 11 June 2020 study from the TUC found a quarter of pregnant women in the UK have faced discrimination at work during the coronavirus outbreak.
The responsibility on employers to assess risks through their supply chains is also absent from WHO’s approach, despite being a concern raised by global unions and ILO, and ITUC calls for ‘due diligence’. Migrant workers, a key affected group in some major work-related outbreaks are also overlooked in the risk assessment considerations.
But even for those jobs recognised by WHO as high risk, the UN agency falls short. Its Q&A recommends “medical masks” alongside other personal protective equipment (PPE) for high risk work. But medical masks do not provide proper protection; respirators of an FFP3/N95 standard should be provided as a minimum.
An Annals of Internal Medicine paper, published on 29 June 2020, noted: “Use of N95 respirators to protect HCWs should not merely be a preference or a recommendation based on availability. The data indicate that it should be the standard for all inpatient Covid-19 management.”
Peg Seminario, an adviser to the US national union federation AFL-CIO, described this WHO guidance as “incredibly harmful” and likely to undermine existing workplace protections.
We know what WHO is doing, we know how WHO is doing it, but it remains a mystery why WHO continues to defend a policy that is neither health-based nor science-based.
But it is becoming increasingly clear who is dying as a result.
Selected references
Q&A: Tips for health and safety at the workplace in the context of COVID-19, WHO, 26 June 2020.
Considerations for public health and social measures in the workplace in the context of COVID-19, WHO, 10 May 2020.
A safe and healthy return to work during the COVID-19 pandemic, ILO policy brief, 22 May 2020.
Key issues on the return to work, ITUC Covid-19 briefing, 15 May 2020.
Fears SC, Klimstra WB, Duprex P, Hartman A, Weaver SC, Plante KS, et al. Persistence of severe acute respiratory syndrome coronavirus 2 in aerosol suspensions, Emerging Infectious Diseases, September 2020 [date cited]. Original publication date: 22 June 2020.
Prateek Bahl, Con Doolan, Charitha de Silva, Abrar Ahmad Chughtai, Lydia Bourouiba, C Raina MacIntyre. Airborne or Droplet Precautions for Health Workers Treating Coronavirus Disease 2019?, The Journal of Infectious Diseases, jiaa189, 16 April 2020.
C Raina MacIntyre and Quanyi Wang. Physical distancing, face masks, and eye protection for prevention of COVID-19, The Lancet, published online 1 June 2020.
Derek K Chu, Elie A Akl, Stephanie Duda, Karla Solo, Sally Yaacoub, Holger J Schünemann, on behalf of the COVID-19 Systematic Urgent Review Group Effort (SURGE) study authors. Physical distancing, face masks, and eye protection to prevent person-to-person transmission of SARS-CoV-2 and COVID-19: a systematic review and meta-analysis, The Lancet, published online 1 June 2020.
Nhu Quyen Dau, Harry Peled, Helen Lau, Julie Lyou, and Claudia Skinner. Why N95 Should Be the Standard for All COVID-19 Inpatient Care, Annals of Internal Medicine, 29 June 2020. https://doi.org/10.7326/M20-2623
Advice on the use of masks in the context of Covid-19, WHO interim guidance, 5 June 2020. Comments from WHO director-general, media briefing, 5 June 2020.
Qin-Long Jing, Ming-Jin Liu, Zhou-Bin Zhang, Li-Qun Fang, Jun Yuan, An-Ran Zhang and others. Household secondary attack rate of Covid-19 and associated determinants in Guangzhou, China: a retrospective cohort study, The Lancet Infectious Diseases, online first, 17 June 2020.
Virginia E Pitzer and Ted Cohen. Household studies provide key insights on the transmission of, and susceptibility to, SARS-CoV-2, The Lancet Infectious Diseases, online first, 17 June 2020.
Keep your distance: Is two metres too far or not far enough to protect from COVID-19 and who benefits and who loses if it is reduced?, Stirling University commentary, 22 June 2020.
Lidia Morawska, Donald K Milton. It is Time to Address Airborne Transmission of COVID-19, Clinical Infectious Diseases, ciaa939, 6 July 2020.
Shin Young Park and others. Coronavirus Disease Outbreak in Call Center, South Korea, Emerging Infectious Diseases, volume 26, number 8, August 2020.
Matthew J Evans. Avoiding Covid-19: Aerosol guidelines, medRxiv preprint, 25 May 2020.
Clive B Beggs. Is there an airborne component to the transmission of COVID-19?: a quantitative analysis study, medRxiv preprint, 25 May 2020.
ONS publication note and analysis of deaths in England and Wales related to Covid-19 by occupation and the occupations in the UK that have the highest potential exposure to Covid-19, 11 May 2020.
Coronavirus (COVID-19) related deaths by occupation, England and Wales: deaths registered between 9 March and 25 May 2020, ONS, 26 June 2020.
Fan-Yun Lan, Chih-Fu Wei, Yu-Tien Hsu, David C Christiani and Stefanos N Kales. Work-related COVID-19 transmission in six Asian countries/areas: A follow-up study, PLoS ONE 15(5): e0233588, 19 May 2020.
DOI:
https://doi.org/10.1371/journal.pone.0233588.
Marissa G Baker, Trevor K Peckham, Noah S Seixas. Estimating the burden of United States workers exposed to infection or disease: A key factor in containing risk of COVID-19 infection. PLOS ONE, volume 15, number 4, 28 April 2020: e0232452
DOI: 10.1371/journal.pone.0232452
Risky business: Economic impacts of the coronavirus crisis on different groups of workers, Resolution Foundation, 28 April 2020.
Understanding the impact of COVID-19 on BAME groups, Public Health England review, 16 June 2020.
Data Brief: Silenced About COVID-19 in the Workplace, NELP, 10 June 2020.
Pregnant and precarious: new and expectant mums’ experiences of work during Covid-19, TUC, 11 June 2020.
Social protection for migrant workers: A necessary response to the COVID-19 crisis, Factsheet, ILO, 24 June 2020.
The effects of Covid-19 on global supply chains, Research brief, ILO, June 2020.
Towards mandatory due diligence in global supply chains, ITUC, 22 June 2020.
Oran DP. Topol EJ. Prevalence of Asymptomatic SARS-CoV-2 Infection: A Narrative Review, Annals of Internal Medicine. 3 June 2020.
Furukawa NW, Brooks JT, Sobel J. Evidence supporting transmission of severe acute respiratory syndrome coronavirus 2 while presymptomatic or asymptomatic, Emerging Infectious Diseases, volume 26, number 7, July 2020.
Lucy Rivett and others. Screening of healthcare workers for SARS-CoV-2 highlights the role of asymptomatic carriage in COVID-19 transmission, CITIID-NIHR COVI Bioresource Collaboration, medRxiv, published online 15 May 2020.
Krystal J Godri Pollitt and others. COVID-19 vulnerability: the potential impact of genetic susceptibility and airborne transmission, Human Genomics volume 14, article number 17, published online 12 May 2020.
Krithi Ravi. Ethnic disparities in COVID-19 mortality: are comorbidities to blame?, The Lancet, Online first 19 June 2020.
Talib Dbouk and Dimitris Drikakis. On coughing and airborne droplet transmission to humans, Physics of Fluids, volume 32, issue 5, published online 19 May 2020.
WHO KNEW?
Who’d have thought we’d have to put a health warning on the World Health Organisation? Hazards editor Rory O’Neill discovered WHO’s ‘incredibly harmful’ advice on workplace Covid-19 risks is leaving workers in mortal danger.

| Contents | |
| • | Miscalculated risk |
| • | Transmission impossible |
| • | Aiming low |
| • | Wrong on risks |
| • | High risk strategy |
| • | WHO, what, how, why? |
| • | Selected references |
| Hazards webpages | |
| • | Hazards news |
| • | Infections |
| • | Work and health |
 See Hazards's dedicated Coronavirus resource pages
See Hazards's dedicated Coronavirus resource pages

